Alzheimer’s disease is a “social epidemic,” a new model of care to reduce the impact on families
About one million Italians affected by dementia, 600.000 those with Alzheimer’s disease; numbers set to double within just 20 years. More than 11 billion euros annually in direct costs of Alzheimer’s care.
The family is increasingly the focus of care, while the supply of services shrinks with deep territorial differentiations: according to the third research recently conducted by Censis and AIMA, only 56.6 percent of patients are cared for by a public facility, while 38 percent of families have to use a caregiver. 40% of caregivers, despite being of working age, are not working, and 80% have direct health consequences.
Attention focused on the need for a new care model and future therapies in the Continuing Professional Education Course “Alzheimer’s Disease, chronicle of a social epidemic. Between therapies and care, beyond clichés,” sponsored by Sapienza University of Rome’s Master’s program “Science in Journalistic Practice” with support from Lilly.
A true health and social “epidemic,” with more than 600.000 thousand patients, set to increase rapidly, and a growing impact on the social and economic system of Italy, Europe’s longest-living country, with 13.4 million people over the age of 60, or 22 percent of the population.
This is the scenario of Alzheimer’s disease, one of the great chronic-degenerative diseases of contemporary societies, which not only impairs the memory and other cognitive faculties of patients, but also absorbs resources, takes away time, and erodes the health and job prospects of caregivers.
This is also confirmed by data from the third research recently conducted by Censis with the AIMA (Italian Alzheimer’s Disease Association): the direct costs of care in Italy amount to more than 11 billion euros, 73% of which are borne by families. The average annual cost per patient is 70.587 euros and includes costs borne by the National Health Service, those borne directly on families indirect costs such as caregiver charges, lost income from work for patients, etc. Families are increasingly taking on the burden of care and supervision, sacrificing health and work: only 56.6 percent of patients are cared for by a public facility, while 38 percent of families have to rely on a caregiver, mostly drawing on their own resources. Faced with an increasingly less sustainable impact, surely it is the entire care model that should be rethought, strengthening the network of services and providing interventions to support the patient and caregivers.
Alongside this synergistic approach, scientific research could play a crucial role, as the discovery of a drug, capable of delaying the patient’s state of loss of self-sufficiency by as little as 5 years, would have a significant impact on social and health care costs.
This is the indication agreed upon by institutional decision-makers, specialists, and representatives of patients and families who met in Rome at the Professional Training Course “Alzheimer’s disease, chronicle of a social epidemic. Between therapies and care, beyond clichés” sponsored by Sapienza University of Rome’s Master’s program ‘Science in Journalistic Practice,’ with the support of Lilly.
“A country’s level of civilization is also measured by its attention to patients with disorders affecting the brain, who require a much more complex level of care than patients with other diseases – says Mario Melazzini, President of AIFA – early intervention, Diagnosing the disease in the early stages by slowing the neurodegenerative process is of paramount importance. In fact, it is estimated that if there is no investment in prevention and treatment, Alzheimer’s disease alone will rise from 36 million cases worldwide today to 115 million by 2050, with a dramatic increase in related health care costs.
AIFA and regulatory agencies around the world are working to act not only on authorization procedures by favoring, for example, adaptive or conditional pathways to allow earlier access to care, but also on scientific advice along all stages of clinical development“.
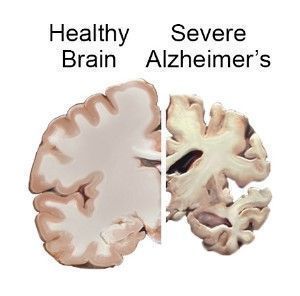
Alzheimer’s disease is degenerative process that consists of the progressive loss of neurons and is manifested by the also progressive decline in memory and other cognitive functions, such as the ability to formulate and understand verbal messages or to perform certain voluntary movements correctly. Age is the main risk factor: the prevalence, which is very low under age 65, increases with age (35 percent at age 80-90). The causes of the disease are unclear, but abnormal deposition of amyloid protein in the brain is established. “Dementia, of which Alzheimer’s accounts for 60-70% of cases, is rightly called an epidemic – says Rossella Liperoti, Geriatrician of the Alzheimer’s Evaluation Unit, University Polyclinic Foundation “A.
Gemelli” of Rome – it is from the health point of view in that the numbers of dementias are dramatically increasing, one million sufferers in Italy alone, and will double in the next two decades, and it is from the social point of view, because Alzheimer’s disease does not only affect the patient, but involves the family and society because of the very high welfare and social costs that fall almost entirely on the family unit, which is poorly supported by services that are very uneven across the country“.
According to the Censis-AIMA survey, the average caregiver devotes 4.4 hours per day of direct care and 10.8 hours of supervision to the Alzheimer’s patient. 40 percent of caregivers, despite being of working age, are not working, and the percentage of unemployed is 10 percent, a threefold increase from just 10 years ago. Caregiver’s commitment also leads to consequences on their health status, particularly among women: 80.3 percent complain of fatigue, 63.2 percent do not get enough sleep, 45.3 percent say they suffer from depression, and 26.1 percent get sick often.
To date, there are no therapies that can prevent or cure Alzheimer’s disease: some drugs are used to relieve certain symptoms such as agitation, anxiety, depression, hallucinations, confusion and insomnia. These drugs are effective for a limited number of patients and for a limited period of time, and may cause undesirable side effects. Drug therapy is complemented by rehabilitation therapies (e.g. occupational therapy, music therapy, etc.) that aim to maintain the patient’s residual abilities for as long as possible.
Although much research is under way and significant progress has been made in pharmacological research, we still do not have a cure capable of modifying the natural history of the disease, halting or slowing down the degenerative process: this is what the so-called “experimental” therapies – developed and studied by several pharmaceutical companies – such as those that act directly on the mechanisms involved in the accumulation of beta-amyloid.
“The contribution of research lies in two words: “the cure,” which will block or slow down the disease – says Paolo Maria Rossini, director of the Institute of Neurology at Policlinico “Gemelli” in Rome – remember that Alzheimer’s is a multifactorial disease, and researchers are working on multiple strands with molecules that can counteract beta-amyloid, Tau protein, oxidation processes, heavy metals such as free copper. Eventually, as happened with AIDS, we will not have a single effective drug but a cocktail of drugs geared toward potential targets. The crucial point, however, is another: we need a paradigm shift in identifying potential sufferers; in fact, this disease is established at least 20 years before the appearance of initial symptoms; the brain is able to counteract it for a long time“.
Pharmacological research, however, is only one aspect of the integrated response needed to face the challenge of Alzheimer’s disease: equally important is to develop a possible management model for the disease and its social and health repercussions, to arrive at an adequate pathway so that patients and caregivers are no longer left alone.
“Don’t forget those who forget” is the slogan that summarizes the commitment deployed in this direction by the Italian Alzheimer’s Disease Association, which, in addition to offering support to patients and caregivers, is engaged in a reflection on the welfare system, to “invent” solutions, suggest and propose modifications and changes to protect patients and family members.
“Data from the third survey carried out by Censis with AIMA, which analyzed the evolution over the past 16 years of the condition of Alzheimer’s patients and their families, confirm the burden not only psychological and social but also economic burden on families: this makes it even more urgent to build a territorial network of appropriate services to support families in the long journey of the disease – explains Patrizia Spadin, AIMA president – unfortunately, in our country, only a few regions offer real integration between health and care, which puts the patient and the family at the center of a virtuous and competent network“.
In short, if the scenario looms dramatically, there is no shortage of models and good practices in Italy that can be replicated to address the current and future emergency. To make them concrete, however, requires the synergistic commitment among all actors aimed at a strategy of sustainable actions that can improve the quality of life of patients and their caregivers: from prevention to certain diagnosis, from pharmacological treatments to the care pathway appropriate to the needs.